CYSTERS – if you’ve had a painful hysteroscopy – recently or in the past – this anonymous survey is for YOU.
The Campaign Against Painful Hysteroscopy compiled the survey. We’re a community group of several hundred women who’ve all had shockingly painful NHS outpatient gynae experiences. We run a public Facebook page, plus a private FB Action/Support Group, which welcomes anyone who’s had a painful hysteroscopy. On Twitter we’re @HysteroscopyA
Unfortunately, the (predominantly) male gynae policy-Tsars at the Department of Health, notably Professor Sean Duffy, are on record as stating that ‘too much emphasis’ is placed on painful hysteroscopy. One leading hysteroscopist claims that severe pain is in fact a ‘rare occurrence’. Lyn Brown, MP’s speeches and debate in the House of Commons about painful hysteroscopy are apparently the result of a ‘misconception’. Hmm. Hysteroscopy without a pre-op assessment or the help of an anaesthetist is a well-known Cash Cow for the NHS. Yes, those silly women will be too embarrassed and/or shocked to complain. It’s not really a problem. No-one dies. Except possibly those women too traumatised to return for gynae cancer diagnosis or treatment. But no-one makes that connection.
Our survey is designed to quantify the causes, circumstances and long-term Patient Report Outcomes of acute hysteroscopy pain – our ‘dirty little secret’.
We’re hoping that your responses could persuade the Department of Health to insist clinics offer all womb endoscopy patients an individual choice of IV sedation/general anaesthetic/epidural/Entonox/stronger painkillers rather than Trial by ‘vocal local’ and ibuprofen.
Yes, you read that right. The NHS routinely offers colonoscopy patients IV sedation. But hysteroscopy patients typically only get OTC meds and ‘distraction technique’ when doctors pass a metal rod passed through the cervix and into the uterus then remove tissue. Nurses then supply tea and (sometimes biscuits) for shock.

According to the British Society for Gynaecological Endoscopy (BSGE) ‘women prefer outpatient hysteroscopy’ to general anaesthetic. This statement is almost certainly true if an outpatient hysteroscopy with no anaesthetic is performed by one of the excellent, highly skilled teams on a pre-screened, healthy pre-menopausal woman who’s given birth vaginally. But in the bog-standard, cash-strapped general hospital Trial by Outpatient Hysteroscopy is the default test for all women needing investigation of the womb. Interestingly, some gynaecologists still assert that there are no functioning nerve fibres in the cervix or uterus! This year’ BSGE conference debated the motion: “Neuropelveology – a fuss about nothing?” Don’t ask which side won!
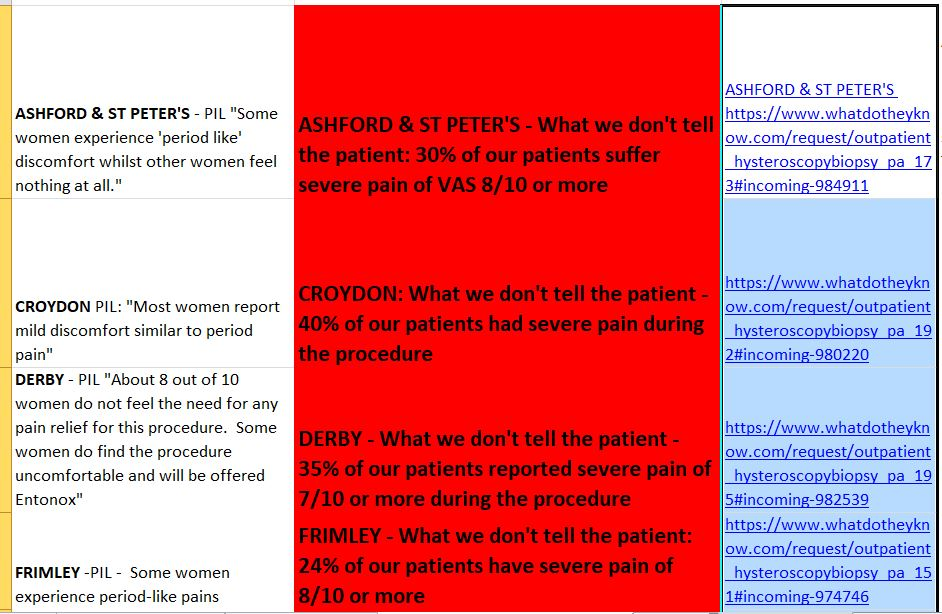
Our campaign has used the Freedom of Information Act to obtain NHS pain-audits. These show that 75% of hysteroscopy patients experience nothing more than short-lived moderate pain. Some people don’t feel a thing. But 25% report severe pain on a VAS scale of 7/10 or more. A proportion of these patients go on to develop PTSD.
Here’s a typical story from one of our group members. Sadly, comments on our Change.Org petition https://www.change.org/p/secretary-of-state-for-health-end-barbaric-nhs-hysteroscopies-with-inadequate-pain-relief show that this story is far too common. This patient should never have undergone Trial by Outpatient Hysteroscopy:
I went for a hysteroscopy and biopsy. I was sent after suffering 2 week long heavy periods. My GP told me it was an outpatient clinic and it was nothing to worry about, ‘just like a smear test’.
I suffer with fibromyalgia and had significant anxiety about the appointment. Once I was called through to the procedure room I was instructed to remove my underwear and hitch up my skirt, place my legs on the supports and relax. The consultant didn’t even make eye contact with me. The nurse stood by my side like a statue. I wasn’t offered any comfort or reassurance despite my obvious distress. Then it began. I was filled inside with water, as the doctor started I screamed out in pain and sobbed. My uterus started contracting and I felt like I was in labour. At no point did they offer to stop. The nurse said and did nothing. Then they attempted to insert the camera and I nearly hit the ceiling. It was searing agony. I have never given birth vaginally, I had 2 c sections. I have never felt pain like it and I felt like I was going to pass out. The doctor then said as I was making such a fuss, they would use a local anesthetic on my cervix which they promptly injected. I sobbed and sobbed. This felt like medieval torture. They then tried the camera again. It was still agony, I bit down and cried. I was told to hold still and it would be over soon.
The doctor said it all looked normal inside and that a coil would sort my problem out. Before I could even think about it they had shoved a coil in me that I didn’t really want and then I was told to go get my underwear back on. I could barely move, I think i was in shock, I felt sick, faint and in disbelief that this was happening to me. I then got up and felt wet as water ran down my legs, not just water as I discovered it was mixed with my blood. It was all over my skirt, it had run off of the seat and all over the floor like a horror scene. I was told to use a sanitary towel if I had bleeding so I took one of the giant ones offered.
That was it, I was sent out to go home. I called my husband to collect me and I cried my eyes out. When I got home and got out of the car I realised I had bled straight through the towel, my clothes and all over the car seat. As the afternoon went on I felt worse and worse. I felt like a wreck and like I had just been tortured.
I am still petrified of having my next smear, I dread the time that this coil needs to be removed because I don’t think I can let them near me again. I will never trust a doctor when they say something is simply ‘uncomfortable’
I still think about it and have flashbacks of that pain.
So thank you CYSTERS – any help you can give in sharing our survey will be deeply appreciated by future patients.



